PRP for back pain is one of the most searched regenerative treatments in the US right now, and for good reason. Back pain is the leading cause of disability worldwide, affecting roughly 60 to 80 percent of adults at some point in their lives. Most of them cycle through the same options: anti-inflammatories, steroid injections, physical therapy, and eventually surgery. PRP offers a different path — one that works with your body’s own biology instead of temporarily masking the problem.
This article breaks down exactly what PRP injections do for back pain, which types of back pain respond best, what the procedure involves, and what you should realistically expect from results.
What PRP Actually Does Inside Your Spine
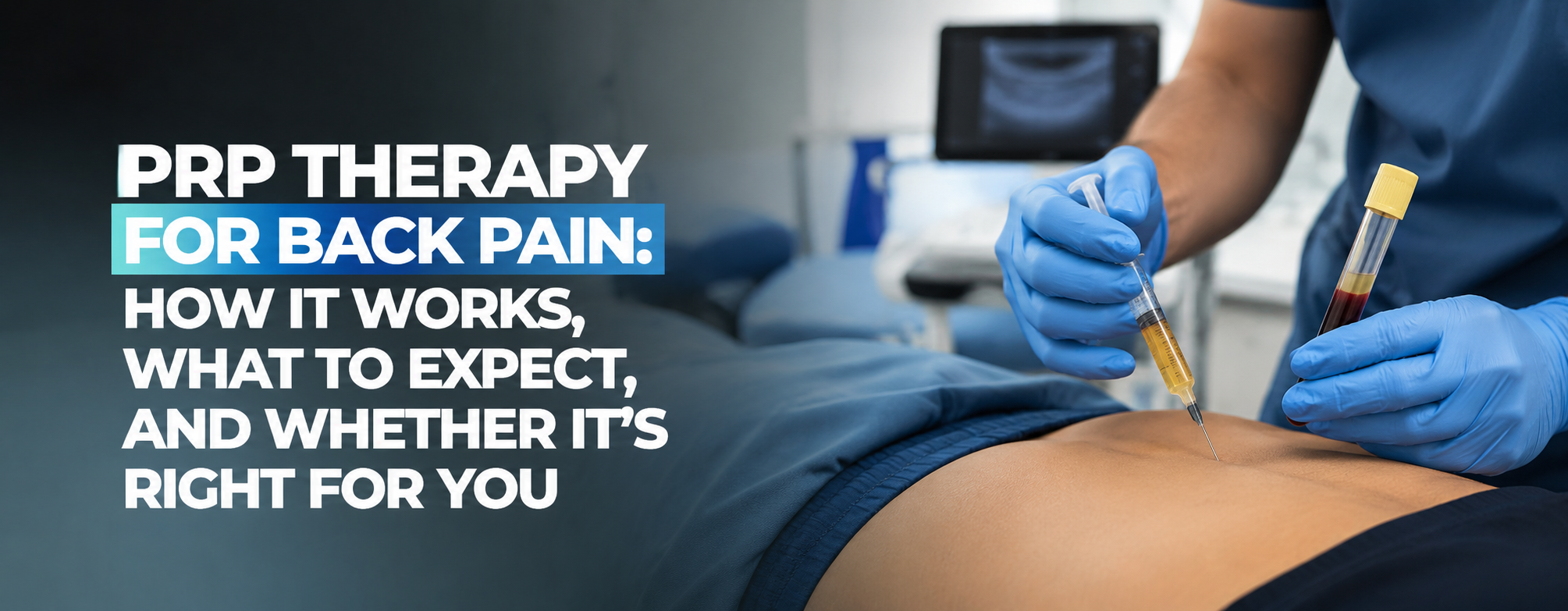
Platelet-Rich Plasma starts with a small blood draw from your arm. That blood gets spun in a centrifuge to concentrate the platelets — the components of your blood that carry growth factors and signaling proteins. The resulting solution contains anywhere from 5 to 10 times the normal concentration of platelets found in whole blood.
When that concentrated solution gets injected into the damaged area of your spine, those growth factors trigger something your body already knows how to do but often can’t do efficiently in spinal tissue: repair. Spinal discs, facet joints, and the ligaments surrounding the lumbar spine have poor blood supply compared to muscles and skin. That’s exactly why back injuries heal slowly — the healing signals can’t reach the damage at sufficient intensity. PRP delivers those signals directly where they’re needed.
The growth factors in PRP stimulate collagen production, reduce local inflammation, and activate any remaining healthy cells in the damaged tissue to regenerate. For degenerative disc disease specifically, studies have shown PRP can help restore disc height and hydration — structural improvements that steroids simply cannot produce.
Which Types of Back Pain Respond to PRP
Not all back pain is the same, and PRP isn’t the right tool for every type. The conditions that respond best are those involving damaged or degenerated soft tissue and joints — precisely the structures that PRP’s growth factors can reach and repair.
Degenerative disc disease is one of the strongest candidates. When the discs between vertebrae break down with age or wear, they lose height and hydration, causing pain and stiffness. PRP injected directly into the disc has shown significant pain reduction and functional improvement in clinical trials, with one 48-week study reporting 71 percent of patients classified as treatment successes.
Sacroiliac (SI) joint pain is another area where PRP consistently outperforms steroid injections. The SI joint is a major cause of lower back pain that often gets misdiagnosed as a pinched nerve or sciatica. Physicians at Ohio State’s Spine Care program use PRP specifically for SI joint pain, citing longer-lasting benefits compared to steroids that may only last a few weeks or months.
Facet joint arthropathy — the breakdown of the small joints along the back of the spine — also responds well to PRP. Research from the University of Oklahoma and Louisiana State University found well-designed studies demonstrating efficacy of PRP for lumbar facet joint injections, with results showing both safety and long-term effectiveness compared to steroid-based approaches.
PRP also works for chronic back and neck pain from ligament laxity, soft tissue injuries, and post-surgical back pain where the original procedure didn’t resolve the underlying problem. It’s particularly useful for patients who’ve gotten temporary relief from steroid injections but keep coming back because the relief doesn’t last.
Where PRP is less indicated: acute fractures requiring structural stabilization, severe nerve compression requiring surgical decompression, and advanced spinal instability. A proper evaluation with imaging is the only way to confirm whether your specific case is a good candidate.
PRP vs. Steroid Injections for Back Pain
Steroid injections (corticosteroids) reduce inflammation fast. If you’ve had one, you know the drill — significant relief for a few weeks, maybe a couple of months, then the pain comes back. That’s because steroids don’t repair anything. They suppress the inflammatory response temporarily, which provides symptom relief, but the underlying tissue damage remains untouched.
PRP works more slowly but addresses the actual cause. The growth factors in PRP don’t just quiet inflammation — they initiate tissue repair. Studies comparing PRP to epidural steroid injections for disc-related lower back pain found that PRP provided sustained relief while the steroid group saw pain return after a few weeks.
There’s also a cumulative risk issue with repeated steroid injections. Corticosteroids can weaken tendons and ligaments with repeated use, and they’re not recommended more than three to four times per year. PRP carries none of those long-term risks because it uses your own blood — there’s no foreign substance and no hormonal effect on the rest of your body.
The tradeoff is that PRP takes longer to work. Most patients notice meaningful improvement four to eight weeks after the injection, as the tissue repair process takes time. If you need acute pain relief right now, that delay matters. If you’re tired of temporary fixes and want actual healing, PRP is the stronger long-term option.
What to Expect During and After a PRP Injection
The procedure itself takes about 45 to 60 minutes from blood draw to injection. After drawing a small blood sample — typically 15 to 60 milliliters from your arm — the sample spins in a centrifuge for about 10 to 15 minutes to concentrate the platelets. The resulting PRP is then loaded into a syringe.
For spinal injections, imaging guidance — usually fluoroscopy (real-time X-ray) or ultrasound — is used to ensure precise needle placement. Accuracy matters significantly here: the closer the injection gets to the actual site of damage, the better the outcome. This is a step that separates experienced regenerative medicine physicians from less rigorous providers.
After the injection, expect soreness at the injection site for one to seven days. This is a normal inflammatory response — the PRP is activating the healing process, and some temporary discomfort is part of that. Most patients return to light daily activities within a day or two. Avoid anti-inflammatory medications (NSAIDs like ibuprofen) for at least two weeks before and after the injection, as they can interfere with the platelet activity that makes PRP work.
Results typically become noticeable between four and eight weeks post-injection, with continued improvement over the following months as tissue repairs. Most patients require one to three sessions, spaced four to six weeks apart, depending on the severity of the condition and the response to initial treatment.
Who Is and Isn’t a Candidate for PRP Back Injections
PRP therapy works best for patients who:
- Have chronic back pain from disc degeneration, facet joint damage, SI joint dysfunction, or ligament injuries
- Have gotten only temporary relief from steroid injections and physical therapy
- Want to avoid surgery or are not surgical candidates
- Have post-surgical back pain that hasn’t resolved
- Are not currently on anticoagulation therapy or can temporarily discontinue it
PRP is generally not appropriate for patients with active cancer, active infection, certain blood disorders, or platelet dysfunction conditions. Age alone is not a disqualifier — PRP therapy works across a wide age range.
The best way to determine candidacy is a thorough evaluation that includes a review of your imaging (MRI or X-ray), a physical exam, and a detailed history of previous treatments. At our clinic in Orlando, Dr. Manuel Colón and Dr. Dana Kleinman conduct this evaluation before recommending any treatment — including ruling out conditions that need surgical intervention first.
PRP for Back Pain in Orlando
If you’re in the Orlando or Lake Nona area and have been managing back pain with temporary solutions that keep wearing off, PRP therapy may be worth a serious conversation. Our team has treated patients with disc degeneration, SI joint pain, facet arthropathy, and chronic lumbar pain who had exhausted conservative options and were facing surgery as the next step.
We also combine PRP with other regenerative approaches when the case warrants it — including stem cell therapy, prolozone therapy, and shockwave therapy — to build a treatment plan based on your actual diagnosis, not a one-size-fits-all protocol.
Contact our team to schedule a consultation. Bring your most recent imaging if you have it. We’ll review everything and tell you directly whether PRP is the right option for your specific condition.
You can also read more about how stem cell therapy helps with back pain, compare PRP vs stem cells to understand which approach fits your case, or see how PRP compares to cortisone in detail.
Frequently Asked Questions
Does PRP work for back pain?
Yes, for specific types of back pain. Clinical evidence consistently shows PRP reduces pain and improves function in patients with degenerative disc disease, sacroiliac joint dysfunction, and facet joint arthropathy. A 48-week clinical trial found 71 percent of patients with discogenic low back pain classified as treatment successes after intradiscal PRP injections. That said, PRP is not effective for all types of back pain — structural problems like severe nerve compression or spinal instability may need a different approach. The right candidate selection is what determines outcomes.
How many PRP injections do you need for back pain?
Most patients need one to three sessions, spaced four to six weeks apart. Mild or more acute conditions may respond to a single injection. Chronic conditions involving significant disc degeneration or multiple affected joints typically require two to three rounds. Your provider should monitor your response after each session and adjust accordingly — a protocol that calls for six sessions upfront without evaluating your progress is a red flag.
How long does PRP pain relief last for back pain?
Relief from PRP injections for back pain typically lasts six months to over a year, and often longer when the underlying tissue has actually repaired. This is a significant difference from steroid injections, which provide relief for weeks to a few months at most. Because PRP promotes actual tissue regeneration rather than just inflammation suppression, results tend to be more durable. Some patients require a maintenance injection every 12 to 18 months; others do not.
How much does PRP therapy for back pain cost?
PRP therapy for back pain typically costs between $500 and $2,500 per session, depending on the provider, the specific injection technique, and whether imaging guidance is used. Most insurance plans do not cover PRP because it’s still classified as investigational for spinal conditions. Some auto insurance or workers’ compensation cases do provide coverage — it depends on your specific situation. We recommend asking about this during your consultation rather than assuming either way.
Is PRP better than steroid injections for back pain?
For long-term outcomes, yes. Steroid injections reduce inflammation quickly but don’t repair the underlying tissue — pain typically returns within weeks to months. PRP works more slowly but triggers actual tissue repair, producing more durable results. Studies comparing PRP to epidural steroids for disc-related lower back pain found PRP provided sustained relief while steroid effects faded. PRP also carries fewer long-term risks than repeated corticosteroid injections, which can weaken spinal ligaments and tendons over time.
What types of back pain does PRP treat?
PRP is most effective for back pain caused by degenerative disc disease, sacroiliac joint dysfunction, facet joint arthropathy, ligament laxity, and soft tissue injuries around the lumbar spine. It’s also used for patients with persistent pain after back surgery. It’s less suited for acute fractures, severe nerve compression requiring surgical decompression, or advanced spinal instability. An MRI and physical evaluation are the starting point for determining which category your back pain falls into — and whether PRP is the right tool for it.